The ideal dental treatment is the one that offers the greatest number of benefits while simultaneously creating the least drawbacks or negative side effects. Why should the choice of crown material be any different?
The ideal crown material has all of the right properties to make it look undetectable amongst the adjacent teeth, unmatched durability, restoration of function, easy cleanability, and does not harm the patient. Zirconia meets all of these requirements and has become the crown material of choice of many dental professionals since the early 2000s.
The Zirconia Crown Difference
Aside from titanium, no other substance used in dentistry is as biocompatible or chemically inert as zirconia. Unlike other restorations that contain a metal substructure, virtually no one is allergic to zirconia. Restorations made from it possess no visible dark lines or shadows that make obtaining an ideal color match difficult. Zirconia is extremely strong on its own without having the bulky appearance that is characteristic of fired porcelain. It is wear-resistant and stands up to bruxism. Clinicians appreciate that crowns and bridges made from zirconia are well-retained by the natural tooth structure using resin ionomer dental cements.
What Is Zirconia?
Zirconia is the perfect material for CAD/CAM manufacturing. It is formed into void-free solid blocks that can be milled into a precise shape without needing another material to create stability and rigidity. Once the shape is formed, it is baked at ultra-high temperatures to produce a finished crown that is nearly indestructible.
What Makes Zirconia So Strong?
The strength of ISO- and ADA-approved monolithic zirconia, a.k.a. Zirconium (IV) oxide, is derived from its tetragonal crystalline properties. When comparing it to glass ceramics and dental composites, zirconia is more split-resistant, stiffer, and stronger. Its strength can be both an asset and a drawback: you may face a challenge when removing a zirconia crown because of its tremendous strength. Trying to cut through a zirconia crown to create endodontic access can be quite challenging.
Zirconia Now Looks Better Than Ever
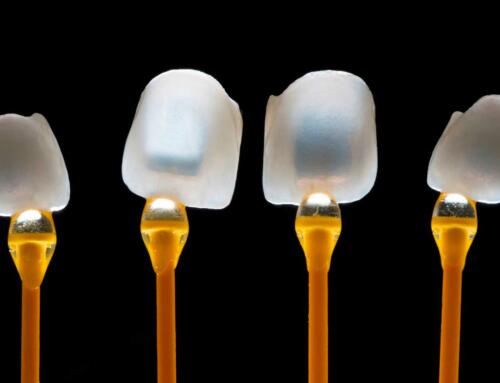
The biggest problem with a full-contour monolithic zirconia crown is the opaque white appearance caused by structural defects that absorb light rather than allow it to pass through. This property is great for hiding discolored tooth structures or core buildups. But since it does not possess all of the translucent and refractory properties that would be desirable for a natural, lifelike appearance, its uses are limited to implant abutments, fabricating non-metal bridge frameworks, and restoring posterior teeth. How do you make zirconia suitable for aesthetically-pleasing anterior restorations? Now it is possible to fabricate zirconia restorations using layered, highly translucent zirconia formulations to create a look that blends with any neighboring tooth or restoration.
How Long Do Zirconia Crowns Last?
Since zirconia has only been in widespread use for roughly fifteen years, no studies compare its longevity to other tried-and-true materials such as gold or porcelain fused-to-metal (PFM). One study by Clinicians Report Foundation spanning nearly 10 years of use on single zirconia crowns made from BruxZir 3Y (manufactured by Glidewell Direct) has shown almost no failures.
However, issues with zirconia crowns leading to their diminished longevity are starting to be noticed by clinicians. In a 2022 article, renowned researcher Gordon J. Christensen delves into this topic and identifies some reasons for zirconia crown failure. These include the lack of adequate tooth preparation, the internal surface of the crown being too smooth or unretentive, crown margins with recurrent decay, open contacts, and zirconia crowns made from zirconia formulations that deviate from the original Glidewell formula. The latter issue has been a large enough reason for failure that Christensen recommends that the dentist should “ask the lab technician what type of zirconia they are using. They should know the answer to that question. If they do not, find another lab that does know what they are using.”
Like any gold or PFM crown, zirconia crowns are strong only when they are of sufficient thickness. Lack of adequate tooth reduction will cause a less-than-desirable result and make it impossible for the dental laboratory technician to provide an aesthetically-pleasing crown that will last for years. Gingival margins should be at a minimum of 0.6 mm deep. The axial walls of the preparation must be at least 1.0 mm in depth, and occlusal reduction of at least 1.5 mm should follow the original tooth’s anatomy. Proper patient home care, including regular brushing, flossing, and maintenance visits, will help to ensure crown longevity.
Zirconia Crowns: The Disadvantages
No dental material is perfect; thus, zirconia crowns can potentially be disadvantages.
Appearance
Originally, only bone-white substructures could be produced for zirconia crowns, frequently creating problems in achieving an aesthetic appearance. That issue has been solved with the use of layering techniques that utilize slightly-altered zirconia formulations or porcelain with refractive and reflective properties that hide the underlying monolithic zirconia base and more closely approximate the look of natural teeth.
Wear on Teeth
Because of the hardness and durability of zirconia, damage and wear to the opposing teeth was a concern that has since been minimized. A 2012 study in the Journal of Dentistry found that “feldspathic porcelain was much more likely than zirconia ceramic to cause wear on the enamel of opposing teeth.”
Zirconia Crowns: The Procedure
Despite the disadvantages, the benefits of zirconia crowns far outweigh the negatives and offer biocompatibility, strength, and longevity that PFM can’t provide. When it comes to crown selection, it is important to choose the best type of zirconia restoration to match the patient’s needs.
Full-contour zirconia is known for its superior strength and is best suited for patients with a heavy bite, bruxism, or even heavy canine guidance. A full-contour translucent zirconia crown is more desirable for areas that need to be visually pleasing yet are subjected to far fewer biting and grinding forces. Porcelain fused-to-zirconia (PFZ) involves fabricating a full-contour zirconia crown. A window on the face of the crown is cut out so as not to compromise the strength of the zirconia. Then, an overlay of translucent porcelain is layered and baked onto the surface. External stains are applied for characterization with incredible results. PFZ is the ultimate combination of both wear resistance and aesthetics.
Zirconia Crowns from Stomadent Dental Lab
The best crown is the one that restores and provides a function that nobody notices. Trust the expert technicians at Stomadent Dental Laboratory to fabricate the ideal aesthetic zirconia restoration using their completely automated digital workflow that eliminates defects and preserves contacts and occlusion, saving you the time and aggravation of numerous chairside adjustments. See all of the great-looking zirconia restorations that Stomadent has to offer today!